Vulva
| Human vulva | |
|---|---|
|
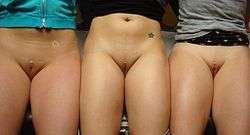
Vulvae of different women (pubic hair removed in some cases) (Genetic variation) | |
| Details | |
| Precursor | Genital tubercle, urogenital folds |
| Artery | Internal pudendal artery |
| Vein | Internal pudendal veins |
| Nerve | Pudendal nerve |
| Lymph | Superficial inguinal lymph nodes |
| Identifiers | |
| Latin | pudendum femininum |
| MeSH | 05.360.319.887 |
| TA | A09.2.01.001 |
| FMA | 20462 |
The vulva (Latin: wrapper, covering, plural vulvae or vulvas)[1] consists of the external genital organs of a woman.[2] The vulva includes the mons pubis, labia majora, labia minora, clitoris, bulb of vestibule, vulval vestibule, urinary meatus, greater and lesser vestibular glands, and the vaginal opening.[3][4] The urinary meatus is also included as it opens into the vulval vestibule. Other features of the vulva include: the pudendal cleft, sebaceous glands, the urogenital triangle (anterior part of the perineum), and pubic hair.
As the vulva is the gateway to the uterus (womb), a double layer of protection is provided by the folds of the outer and inner labia. The vulva can be affected by many disorders which can often result in itching. Vulvovaginal health measures can prevent many of these.[2]
Structure

Structures and features
The main structures of the vulva are: the mons pubis, the labia (majora and minora) including the frenulum, the external part of the clitoris, the urinary meatus, the vaginal opening and hymen, and the greater and lesser vestibular glands.
Other features include: the pudendal cleft, sebaceous glands, the vulval vestibule, and the urogenital triangle (anterior part of the perineum).
The soft mound at the front of the vulva is formed by fatty tissue in the pubic region covering the pubic bone, and is called the mons pubis. Mons pubis is Latin for "pubic mound" and is present in both sexes. Sometimes a variant term is used specific to women—the mons veneris ("mound of Venus"). The mons pubis separates into the labia —two pairs of folds of tissue that protect the vulvar vestibule.
The outer pair of folds are the labia majora, (New Latin: larger lips). The labia majora are divided by the pudendal cleft and they contain and protect the other, more delicate structures of the vulva. The labia majora meet again at the urogenital triangle (the anterior part of the perineum) between the pudendal cleft and the anus. The color of the outside skin of the labia majora is usually close to the overall skin color of the individual, although there is considerable variation. The inside skin and mucus membrane are often pink or brownish.

The labia minora (smaller lips) are the inner two soft folds of the labia, within the labia majora, and contain numerous sebaceous glands.[5] Though called the smaller lips they can often be of considerable size, and may protrude outside the labia majora. Much of the variation among vulvas lies in the significant differences in the size, shape, and color of the labia minora. This variation has also been evidenced in a large display of 400 vulval casts called the Great Wall of Vagina created to fill the lack of information of what a normal vulva looks like. The casts taken from a large and varied group of women showed clearly that there is much variation.[6]
The clitoris is located at the front of the vulva, where the labia minora meet. The visible portion of the clitoris is the clitoral glans. Typically, the clitoral glans is roughly the size and shape of a pea, although it can be significantly larger or smaller. The clitoral glans is highly sensitive, containing as many nerve endings as the homologous organ in males, the glans penis. The point where the labia minora attach to the clitoris is called the frenulum clitoridis. A prepuce, the clitoral hood, normally covers and protects the clitoris, however in women with particularly large clitorises or small prepuces, the clitoris may be partially or wholly exposed at all times. The clitoral hood is the female equivalent of the male foreskin. Often the clitoral hood is only partially hidden inside of the pudendal cleft.
The area between the labia minora is called the vulval vestibule, and it contains the vaginal opening and the urinary meatus. The urinary meatus is located below the clitoris and just in front of the vagina.
The opening of the vagina is located at the bottom of the vulval vestibule, toward the perineum. The term introitus is more technically correct than "opening", since the vagina is usually collapsed, with the opening closed, unless something is inserted. The introitus is sometimes partly covered by a membrane called the hymen. The hymen will usually rupture during the first episode of vigorous sex, and the blood produced by this rupture has been seen as to signify virginity. However, the hymen may also rupture spontaneously during exercise (including horseback riding) or be stretched by normal activities such as use of tampons and menstrual cups, or be so minor as to be unnoticeable. In some rare cases, the hymen may completely cover the vaginal opening, requiring surgery.
On either side of the back part of the vaginal opening are the two greater vestibular glands also known as Bartholin's glands. These glands secrete mucus and a vaginal and vulval lubricant.[7] They are homologous to the bulbourethral glands in the male.The lesser vestibular glands also known as Skene's glands, are found on the anterior wall of the vagina. They are homologues of the male prostate gland and are also referred to as the female prostate.[8]
The skin of the vulva is more delicate than other areas of skin.[9]Pubic hair is much coarser than other body hair. It appears at puberty and is considered a secondary sex characteristic.[10][11] The mons pubis and the labia majora become covered by pubic hair and it can also grow on the inner thighs and perineum. Pubarche is the first appearance of pubic hair and can occur independently of puberty. Premature pubarche may indicate underlying endocrine conditions.[12] Apocrine sweat glands secrete sweat into the pubic hair follicles. This is broken down by bacteria on the skin and produces an odor,[13] which some consider to act as a sex pheromone (sexual attractant).
The tissues of the vulva are highly vascularised and blood supply is provided by the three pudendal arteries. Venous return is via the external and internal pudendal veins. The organs and tissues of the vulva are drained by a chain of superficial inguinal lymph nodes located along the blood vessels.[4][10]
Nerve supply
The ilioinguinal nerve originates from the first lumbar nerve and gives branches that include the anterior labial nerves which supply the skin of the mons pubis and the labia majora. The perineal nerve is one of the terminal branches of the pudendal nerve and this branches into the posterior labial nerves to supply the labia. The pudendal nerve branches include the dorsal nerve of clitoris which gives sensation to the clitoris.
The pudendal nerve enters the pelvis through the lesser sciatic foramen and continues medial to the internal pudendal artery. The point where the nerve circles the ischial spine is the location where a pudendal block of local anesthetic can be administered to inhibit sensation to the vulva. A number of smaller nerves split off from the pudendal nerve. The deep branch of the perineal nerve supplies the muscles of the perineum and a branch of this supplies the bulb of the vestibule.[4][14]
Muscle tissue

Pelvic floor muscles help to support the vulvar structures.[4] The voluntary, pubococcygeus muscle, part of the levator ani muscle partially constricts the vaginal opening.[11] Other muscles support the vulvar area. These are the transverse perineal muscles, the bulbospongiosus, and the ischiocavernosus muscles.[10] The muscles are part of the urogenital triangle.
Development
Fetus

The appearance of the external genital region is the same for males and females during the eighth week.[15]
Beginning in the third month of development, the genital tubercle becomes the clitoris. The urogenital folds become the labia minora, and the labioscrotal swellings become the labia majora.
Childhood
At birth, the neonate's vulva (and breast tissue—see witch's milk) may be swollen or enlarged as a result of having been exposed, via the placenta, to her mother's increased levels of hormones. The clitoris is proportionally larger than it is likely to be later in life. Within a short period of time as these hormones wear off, the vulva will shrink in size. From then until puberty the vulva doesn't change in appearance, other than growing in proportion with the rest of the body.
Puberty
The onset of puberty produces a number of changes. The structures of the vulva become proportionately larger and may become more pronounced. Coloration may change and pubic hair develops, first on the labia majora, and later spreading to the mons pubis, and sometimes the inner thighs and perineum. The labia minora may grow more prominent and undergo changes in color.[16]
In preadolescent girls, the vulva appears to be positioned further forward than in adults, showing a larger percentage of the labia majora and pudendal cleft when standing. During puberty the mons pubis enlarges, pushing the forward portion of the labia majora away from the pubic bone, and parallel to the ground (when standing). Variations in body fat levels affect the extent to which this occurs.
Post-menopause
During menopause, hormone levels decrease, and as this process happens, reproductive tissues which are sensitive to these hormones shrink in size.The mons pubis, labia, and clitoris are reduced in size in post-menopause, although not usually to pre-puberty proportions.This is a condition called vulval atrophy and the decrease in estrogen can cause pale, itchy or sore skin.[9]
Sexual homology
Most male and female sex organs originate from the same tissues during fetal development; this includes the vulva. The anatomy of the vulva is related to the anatomy of the male genitalia by a shared developmental biology. Organs that have a common developmental ancestry in this way are said to be homologous.
The clitoral glans is homologous to the glans penis in males, and the clitoral body and the clitoral crura are homologous to the corpora cavernosa of the penis. The labia majora, labia minora, and clitoral hood are homologous to the scrotum, shaft skin of the penis, and the foreskin, respectively. The vestibular bulbs beneath the skin of the labia minora are homologous to the corpus spongiosum, the tissue of the penis surrounding the urethra. The greater vestibular glands are homologous to the bulbourethral glands in males.
Function and physiology
The vulva has a sexual function; these external organs are richly innervated and provide pleasure when properly stimulated. There are a number of different secretions associated with the vulva, including urine, sweat, menses, sebum, and secretions from the vestibular glands and vaginal wall. These secretions contain a mix of chemicals, including pyridine, squalene, urea, acetic acid, lactic acid, complex alcohols, glycols, ketones, and aldehydes. During sexual arousal, vaginal lubrication increases. Smegma is a white substance formed from a combination of dead cells, skin oils, moisture and naturally occurring bacteria, that forms in the genitalia. In females it collects around the clitoris and labial folds.[17] It is also found in other mammals
Some women produce aliphatic acids. These acids are a pungent class of chemicals which other primate species produce as sexual-olfactory signals. While there is some debate, researchers often refer to them as human pheromones. These acids are produced by natural bacteria resident on the skin. The acid content varies with the menstrual cycle, rising from one day after menstruation, and peaking mid-cycle, just before ovulation.
Sexual arousal
Sexual arousal results in a number of physical changes in the vulva. Vaginal lubrication begins first. Vulva tissue is highly vascularised; arterioles dilate in response to sexual arousal and the smaller veins will compress after arousal,[4][15] so that the clitoris and labia minora increase in size. Increased vasocongestion in the vagina causes it to swell, decreasing the size of the vaginal opening by about 30%. The clitoris becomes increasingly erect, and the glans moves towards the pubic bone, becoming concealed by the hood. The labia minora increase considerably in thickness. The labia minora sometimes change considerably in color, going from pink to red in lighter skinned women who have not borne a child, or red to dark red in those that have. Immediately prior to orgasm, the clitoris becomes exceptionally engorged, causing the glans to appear to retract into the clitoral hood. Rhythmic muscle contractions occur in the outer third of the vagina, as well as the uterus and anus. Contractions become less intense and more randomly spaced as the orgasm continues. An orgasm may have as few as one or as many as 15 or more contractions, depending on its intensity. Orgasm may be accompanied by female ejaculation, causing liquid from either the Skene's gland or bladder to be expelled through the urethra. The pooled blood begins to dissipate, although at a much slower rate if an orgasm has not occurred. The vagina and vaginal opening return to their normal relaxed state, and the rest of the vulva returns to its normal size, position and color.
Clinical significance
Pruritus vulvae is itching in the vulvar region and is a symptom of many underlying causes. Pubic shaving can result in pseudofolliculitis pubis and folliculitis as well as cuts to the labia and clitoris, and ingrown hairs.[18] Pubic shaving increases the risk of contracting the sexually transmitted viral infection, molluscum contagiosum.[19]
A less common inflammatory disorder is mucosal genital lichen planus. A severe variant of this is vulvovaginal gingival syndrome which can lead to narrowing of the vagina,[20] or vulva destruction.[21]
Vulvodynia
Vulvodynia is chronic pain in the vulvar region. There is no single identifiable cause. A sub-type of this is vulvar vestibulitis but since this is not thought to be an inflammatory condition it is more usually referred to as vestibulodynia. Vulvar vestibulitis usually affects pre-menopausal women.
Infections
_Female%2C_from_a_human_host.jpg)
Vulvar organs and tissues can become infected with different pathogens, or infested by parasites. Any inflammation caused is called vulvitis. Sexually transmitted infections may cause signs and symptoms on the vulva even though the agents may not be visible in the vulvar region. Vulvovaginal health measures can help to prevent many disorders.[22]Vaginitis can have many causes and different health measures can help its prevention. The following infections include those that can also be classed as sexually transmitted infections. Infections of the vagina such as vaginosis and of the uterus may produce vaginal discharge which can be an irritant when it comes into contact with the vulvar tissue, causing itching, inflammation and discomfort.[23][24] Bacterial infections include: Chancroid caused by Haemophilus ducreyi; Granuloma inguinale caused by Klebsiella granulomatis; Syphilis caused by Treponema pallidum; and Gonorrhea caused by the bacterium Neisseria gonorrhoeae.
Viral infections include genital herpes caused by the herpes simplex virus (1 and 2), transmissible with or without visible blisters; the lentivirus HIV (human immunodeficiency virus)—transmissible in venereal fluids, semen, breast milk, and blood; HPV (Human papillomavirus)—skin and mucosal contact. 'High risk' types of HPV can cause vulvar cancer.[25][26] Some other types of HPV cause genital warts. Molluscum contagiosum caused by a poxvirus (molluscum contagiosum virus MCV) transmissible on close contact.
A common fungal infection, commonly known as thrush is vaginal yeast infection a type of candidiasis caused by a number of species of Candida.
Parasitic infections include trichomoniasis, pediculosis pubis and scabies. Trichomoniasis is a microparasitic infection caused by the protozoan Trichomonas vaginalis. This is the most common vulval infection (in industrialised societies) and is transmitted by sexual contact.
Pediculosis pubis commonly called crabs, is a disease caused by the ectoparasite crab louse (Pthiras pubis).
Scabies also known as the seven year itch is caused by another ectoparasite, the mite Sarcoptes scabiei usually transmitted by skin to skin contact.
Cancer
Many malignancies can develop in vulvar structures.[4] Most vulvar cancers are squamous cell carcinomas and are usually found in the labia particularly the labia majora.[27] The second most common vulval cancer (though not very common) is vulval melanoma.[28] A vulvectomy may need to be performed in order to remove some or all of the vulva. This procedure is usually performed as a last resort in certain cases of cancer,[29] vulvar dysplasia or vulvar intraepithelial neoplasia.[30]
Signs and symptoms can include: itching, or bleeding; skin changes including rashes, sores, lumps or ulcers, and changes in vulval skin coloration. Pelvic pain might also occur.[31]
Other
- Crohn's disease of the vulva[32]
- Paget's disease of the vulva
- hormone fluctuations
- psoriasis[33]
- lichen sclerosus
- lichen simplex chronicus[33]
- eczema (uncommon)[33]
- seborrheic dermatosis [uncommon))[33]
- papillary hidradenoma
Childbirth
The vulvar region is at risk for trauma during childbirth.[34] During childbirth, the vagina and vulva must stretch to accommodate the baby's head (approximately 9.5 cm (3.7 in)). This can result in tears known as perineal tears in the vaginal opening, and other structures within the perineum.[35] An episiotomy (a pre-emptive surgical cutting of the perineum) is sometimes performed to facilitate delivery and limit tearing. Perineal tearing or cutting does leave scar tissue.
No advantages have been demonstrated in the shaving of pubic hair prior to childbirth. Rates of complications remain the same between women who were shaved and those unshaven.[36][37]
Surgery
Genitoplasties are surgical procedures that can be carried out to repair, restore or alter vulvar tissues, particularly following damage caused by injury or cancer treatment. These procedures include vaginoplasty which can also be performed as a cosmetic surgery. Other cosmetic surgeries to change the appearance of external structures include labiaplasties.
Elective vulvar surgery has been criticized by clinicians.[38][39] The American College of Obstetricians and Gynecologists recommends that women be informed of the risks of these surgeries. They refer to the lack of data relevant to their safety and effectiveness and to the potential associated risks such as infection, altered sensation, dyspareunia, adhesions, and scarring.[40] There is also a percentage of people seeking elective surgery who may be suffering from body dysmorphic disorder and surgery in these cases can be counterproductive.[41]
Society and culture
Many cultures have no or few taboos on exposure of the breasts, but the vulva and pubic triangle are always the first areas to be covered. A Khoisan woman Saartjie Baartman, the so-called "Hottentot Venus" who was exhibited in London at the beginning of the nineteenth century, was paid to display her large buttocks, but she never revealed her vulva.[42] Khoisan women were said to have elongated labia, leading to questions about, and requests to exhibit, their sinus pudoris, "curtain of shame", or tablier (the French word for "apron"). To quote Georges Cuvier, "The labia minora, or inner lips, of the ordinary female genitalia are greatly enlarged in [Khoisan] women, and may hang down three or four inches below the vagina when women stand, thus giving the impression of a separate and enveloping curtain of skin".[43]

The naming of the external genitalia (in both sexes) as pudenda membra (parts to be ashamed of) dates from the mid-17th century.[44] The naming clearly influenced the general perception of the vulva and this is shown in depicted gynaecological procedures. The examiner is adopting the compromise procedure where the woman's genitals cannot be seen.
In some cultures, including modern Western culture, women have shaved or otherwise removed the hair from part or all of the vulva. When high-cut swimsuits became fashionable, women who wished to wear them would remove the hair on either side of their pubic triangles, to avoid exhibiting pubic hair. Other women relish the beauty of seeing their vulva with hair, or completely hairless, and find one or the other more comfortable. The removal of hair from the vulva is a fairly recent phenomenon in the United States, Canada, and Western Europe, usually in the form of bikini waxing or Brazilian waxing, but has been prevalent in many Eastern European and Middle Eastern cultures for centuries, usually due to the idea that it may be more hygienic, or originating in prostitution and pornography. Hair removal may include all, most, or some of the hair. French waxing leaves a small amount of hair on either side of the labia or a strip directly above and in line with the pudendal cleft called a landing strip.
Islam teaching includes Muslim hygienical jurisprudence a practice of which is the removal of pubic hair.[45]
Several forms of genital piercings can be done in the female genital area, and include the Christina piercing, the Nefertiti piercing, the fourchette piercing, and labia piercings. Piercings are usually performed for aesthetic purposes, but some forms like the clitoral hood piercing might also enhance pleasure during sex. Though they are common in traditional cultures, intimate piercings are a fairly recent trend in Western society.[46][47][48]
Altering the female genitalia

The most prevalent form of genital alteration in some countries is female genital mutilation: removal of any part of the female genitalia for cultural, religious or other non-medical reasons. This practice is highly controversial as it is often done to non-consenting minors and for debatable (often misogynistic) reasons. An estimated 100 to 140 million girls and women in Africa and Asia have experienced some form of genital mutilation.[49][50]
Female genital surgery includes laser resurfacing of the labia to remove wrinkles, labiaplasty (reducing the size of the labia) and vaginal tightening. In September 2007, the American College of Obstetricians and Gynecologists issued a committee opinion on these and other female genital surgeries, including "vaginal rejuvenation", "designer vaginoplasty", "revirgination", and "G-spot amplification". This opinion states that the safety of these procedures has not been documented. ACOG recommends that women seeking these surgeries need to be informed about the lack of data supporting these procedures and the potential associated risks such as infection, altered sensation, dyspareunia, adhesions, and scarring.[40]
With the growing popularity of female cosmetic genital surgeries, the practice increasingly draws criticism from an opposition movement of cyberfeminist activist groups and platforms, called the labia pride movement. The major point of contention is that heavy advertising for these procedures, in combination with a lack of public education, fosters body insecurities in women with larger labia in spite of the fact that there is normal and pronounced individual variation in the size of labia. The preference for smaller labia is a matter of a fashion fad and is without clinical or functional significance.[51][52]
Etymology
The word vulva was taken from the Medieval Latin word volva or vulva ("womb, female genitals"), probably from the Old Latin volvere ("to roll"; lit. "wrapper").[53]
Alternative terms
The term pudendum, which denotes the external genitalia, comes from the Latin pudenda membra, meaning parts to be ashamed of.[44] As with nearly any aspect of the human body involved in sexual or excretory functions, there are many slang words for the vulva.[54] "Cunt", a medieval word for the vulva and once the standard term, has become in its literal sense a vulgarism, and in other uses one of the strongest abusive swearwords in English-speaking cultures. Two widespread terms for the vulva, pussy and fanny (in the UK), which used to be a common pet name[55] and nickname[56] respectively, have other non-sexual meanings that lend themselves to double entendres.[57][58][59]
Art


Sheela na gigs are figurative carvings of naked women displaying an exaggerated vulva. They are found in ancient and medieval European contexts. They are displayed on many churches, but their origin and significance is debatable. A main line of thinking is that they were used to ward off evil spirits.
Other cultures have long celebrated and even worshipped the vulva. Some Hindu sects revere it under the name yoni[60] and texts seem to indicate a similar attitude in some ancient Middle Eastern religions.
L'Origine du monde ("Origin of the world") painted by Gustave Courbet in 1866 was the first realistic painting of a vulva to be exhibited in Western art. This example of eroticism is also referenced as inspiring Catherine Breillat's filming of the female genitalia in her 2004 film Anatomie de l'enfer (Anatomy of Hell).[61]
British artist Jamie McCartney used casts of four hundred vulvas to create the installation known as the Great Wall of Vagina in 2011. The vagina casts are life size. Explanations written by the project's sexual health adviser accompany these. The purpose of the artist was to "address some of the stigmas and misconceptions that are commonplace".[62][63][64]
Additional images
 Possible Rupestrian depictions of vulvae, paleolithic
Possible Rupestrian depictions of vulvae, paleolithic- Possible stylised vulva stone, paleolithic
 Attic red-figure lid. Three female organs and a winged phallus.
Attic red-figure lid. Three female organs and a winged phallus. The Universe an oil painting by Meister des Hildegardis-Codex
The Universe an oil painting by Meister des Hildegardis-Codex
References
This article incorporates text in the public domain from the 20th edition of Gray's Anatomy (1918)
- ↑ "vulva". The Free Dictionary. Retrieved 10 April 2016.
- 1 2 Telleen, Steven (11 February 2016). "The Female Reproductive System". Rice University, OpenStax CNX. Retrieved 29 March 2016.
- ↑ Rosdahl, Caroline (2012). Textbook of basic nursing. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 319. ISBN 9781605477725.
- 1 2 3 4 5 6 Hoffman, Barbara; et al. (2011). Williams gynecology (2nd ed.). New York: McGraw-Hill Medical. pp. 794–806. ISBN 9780071716727.
- ↑ Young, Barbra; Lowe, James S; Stevens, Alan; Heath, John W; Deakin, Philip J (March 2006). Wheater's Functional Histology (5th ed.). Elsevier Health Sciences. pp. 175–178. ISBN 978-0-443-06850-8.
- ↑ "'The Great Wall Of Vagina' Is, Well, A Great Wall Of Vaginas (NSFW)". Retrieved 2016-04-17.
- ↑ Lee, MY; Dalpiaz, A; Schwamb, R; Miao, Y; Waltzer, W; Khan, A (May 2015). "Clinical Pathology of Bartholin's Glands: A Review of the Literature.". Current Urology. 8 (1): 22–5. doi:10.1159/000365683. PMC 4483306
 . PMID 26195958.
. PMID 26195958. - ↑ Zaviacic M, Ablin RJ (January 2000). "The female prostate and prostate-specific antigen. Immunohistochemical localization, implications of this prostate marker in women and reasons for using the term "prostate" in the human female". Histol Histopathol. 15 (1): 131–42. PMID 10668204.
- 1 2 "Skin conditions of the vulva". Royal College of Obstetricians & Gynaecologists. Retrieved 6 April 2016.
- 1 2 3 Maclean, Allan; Reid, Wendy (2011). "40". In Shaw, Robert. Gynaecology. Edinburgh New York: Churchill Livingstone/Elsevier. pp. 599–612. ISBN 978-0-7020-3120-5; Access provided by the University of Pittsburgh
- 1 2 Fox, Kent M. Van De Graaff, Stuart Ira (1989). Concepts of human anatomy and physiology (2nd. ed.). Dubuque, Iowa: Wm. C. Brown Publishers. p. 962. ISBN 0697056759.
- ↑ Ibáñez, L; Potau, N; Dunger, D; de Zegher, F (2000). "Precocious pubarche in girls and the development of androgen excess.". Journal of pediatric endocrinology & metabolism : JPEM. 13 Suppl 5: 1261–3. PMID 11117666.
- ↑ "Sweating and body odor Causes - Mayo Clinic". www.mayoclinic.org. Retrieved 16 April 2016.
- ↑ Kyung Won, PhD. Chung (2005). Gross Anatomy (Board Review). Hagerstown, MD: Lippincott Williams & Wilkins. p. 268. ISBN 0-7817-5309-0.
- 1 2 Fox, Kent M. Van De Graaff, Stuart Ira (1989). Concepts of human anatomy and physiology (2nd ed.). Dubuque, Iowa: Wm. C. Brown Publishers. pp. 958–963. ISBN 0697056759.
- ↑ Lloyd, Jillian (May 2005). "Female genital appearance: 'normality' unfolds". British Journal of Obstetrics and Gynecology. 12 (5): 643–646. doi:10.1111/j.1471-0528.2004.00517.x.
- ↑ "Definition of SMEGMA". www.merriam-webster.com. Retrieved 20 April 2016.
- ↑ "Pubic Hair Removal - Shaving". Palo Alto Medical Foundation. Retrieved 2011-11-13.
- ↑ "Risk Factors - Molluscum Contagiosum". CDC. Retrieved 2016-03-24.
- ↑ Panagiotopoulou, N; Wong, CS; Winter-Roach, B (April 2010). "Vulvovaginal-gingival syndrome.". Journal of obstetrics and gynaecology : the journal of the Institute of Obstetrics and Gynaecology. 30 (3): 226–30. doi:10.3109/01443610903477572. PMID 20373919.
- ↑ Schlosser, BJ (May–Jun 2010). "Lichen planus and lichenoid reactions of the oral mucosa.". Dermatologic therapy. 23 (3): 251–67. doi:10.1111/j.1529-8019.2010.01322.x. PMID 20597944.
- ↑ NHS Choices, United Kingdom National Health Service -Preventing vaginal thrush, reviewed 2012-02-17, retrieved June 10, 2013
- ↑ Mastromarino, Paola; Vitali, Beatrice; Mosca, Luciana (2013). "Bacterial vaginosis: a review on clinical trials with probiotics" (PDF). New Microbiologica. 36: 229–238. PMID 23912864.
- ↑ Rimoin, Lauren P.; Kwatra, Shawn G.; Yosipovitch, Gil (2013). "Female-specific pruritus from childhood to postmenopause: clinical features, hormonal factors, and treatment considerations". Dermatologic Therapy. 26 (2): 157–167. doi:10.1111/dth.12034. ISSN 1396-0296.
- ↑ Ljubojevic, Suzana; Skerlev, Mihael (2014). "HPV-associated diseases". Clinics in Dermatology. 32 (2): 227–234. doi:10.1016/j.clindermatol.2013.08.007. ISSN 0738-081X.
- ↑ Zweizig, Susan; Korets, Sharmilee; Cain, Joanna M. (2014). "Key concepts in management of vulvar cancer". Best Practice & Research Clinical Obstetrics & Gynaecology. 28 (7): 959–966. doi:10.1016/j.bpobgyn.2014.07.001. ISSN 1521-6934.
- ↑ UK, Cancer Research. "The vulva". www.cancerresearchuk.org. Retrieved 6 April 2016.
- ↑ UK, Cancer Research. "Types of vulval cancer". www.cancerresearchuk.org. Retrieved 6 April 2016.
- ↑ Fuh KC and Berek JS (2012) Current management of vulvar cancer. Hematol Oncol Clin North Am. 26(1):45-62.
- ↑ Hillemans P, Wang X, Staehle S, Michels W, Dannecker C (2006) Evaluation of different treatment modalities for vulvar intraepithelial neoplasia (VIN): CO(2) laser vaporization, photodynamic therapy, excision and vulvectomy. Gynecol Oncol. 100:271-5.
- ↑ "What Are the Symptoms of Vaginal and Vulvar Cancers?". CDC. 13 March 2014. Retrieved 2016-03-26.
- ↑ Barret, Maximilien; de Parades, Vincent; Battistella, Maxime; Sokol, Harry; Lemarchand, Nicolas; Marteau, Philippe (2014). "Crohn's disease of the vulva". Journal of Crohn's and Colitis. 8 (7): 563–570. doi:10.1016/j.crohns.2013.10.009. ISSN 1873-9946.
- 1 2 3 4 "Vulva — Squamous Hyperplasia". University of Michigan, University of Michigan Health System, Department of Anatomical Pathology, Department of Obstetrics and Gynecology, Division of Gynecological Oncology. Retrieved 25 April 2016.
- ↑ Dudley, Lynn M; Kettle, Christine; Ismail, Khaled MK; Dudley, Lynn M (2013). "Secondary suturing compared to non-suturing for broken down perineal wounds following childbirth". Cochrane Database Syst Rev: CD008977. doi:10.1002/14651858.CD008977.pub2. PMID 24065561.
- ↑ Finn, Martha; Bowyer, Lucy; Carr, Sandra; O'Connor, Vivienne; Vollenhoven, Beverley (2005). Women's Health: A Core Curriculum. Australia: Elsevier. ISBN 0-7295-3736-6.
- ↑ Basevi, Vittorio; Lavender, Tina; Basevi, Vittorio (2014). "Routine perineal shaving on admission in labour". Reviews. doi:10.1002/14651858.CD001236.pub2.
- ↑ Lefebvre, A.; Saliou, P.; Lucet, J.C.; Mimoz, O.; Keita-Perse, O.; Grandbastien, B.; Bruyère, F.; Boisrenoult, P.; Lepelletier, D.; Aho-Glélé, L.S. (2015). "Preoperative hair removal and surgical site infections: network meta-analysis of randomized controlled trials". Journal of Hospital Infection. 91 (2): 100–108. doi:10.1016/j.jhin.2015.06.020. ISSN 0195-6701.
- ↑ Bourke, Emily (2009-11-12). "Designer vagina craze worries doctors". Australian Broadcasting Corporation. Retrieved 5 March 2016.
- ↑ Liao, Lih Mei; Sarah M Creighton (24 May 2007). "Requests for cosmetic genitoplasty: how should healthcare providers respond?". BMJ. British Medical Journal. 334 (7603): 1090–1092. doi:10.1136/bmj.39206.422269.BE. PMC 1877941
 . PMID 17525451. Retrieved 3 March 2016.
. PMID 17525451. Retrieved 3 March 2016. - 1 2 American College of Obstetricians and Gynecologists (2007). "Vaginal "Rejuvenation" and Cosmetic Vaginal Procedures" (PDF): 2. Archived from the original (PDF) on 2008-12-30.
- ↑ Tignol, J; Martin-Guehl, C; Aouizerzate, B (January 2012). "[Body dysmorphic disorder (BDD)].". Presse medicale (Paris, France : 1983). 41 (1): e22–35. doi:10.1016/j.lpm.2011.05.021. PMID 21831574.
- ↑ (Strother 1999)
- ↑ Stuart Ewen; Elizabeth Ewen (4 January 2011). Typecasting: On the Arts and Sciences of Human Inequality. Seven Stories Press. p. 165. ISBN 978-1-58322-949-1.
- 1 2 "pudenda membra". Oxford English Dictionary (2nd ed.). Oxford University Press. September 2005. (Subscription or UK public library membership required.)
- ↑ Ismail, Buyukcelebi (2003). Living in the Shade of Islam: A Comprehensive Reference of Theory and Practice. Tughra Books. p. 169. ISBN 1-932-09921-2.
- ↑ "''Can selfish lovers ever give as good as they get? Plus, the perks of piercings and how to get her to hurry up already''". MSNBC. 2007-12-04. Retrieved 2011-11-13.
- ↑ "Vaughn S. Millner et al. (2005): ''First glimpse of the functional benefits of clitoral hood piercings'',American Journal of Obstetrics and Gynecology, Volume 193, Issue 3, Pages 675-676". Ajog.org. Retrieved 2011-11-13.
- ↑ "VCH Piercings, by Elayne Angel, Seite 16-17, The Official Newsletter of The Association of Professional Piercers" (PDF). Retrieved 2011-11-13.
- ↑ "Female genital mutilation". World Health Organization (WHO). February 2010.
- ↑ "Female genital mutilation". World Health Organization. 2016. Retrieved 2016-03-24.
- ↑ Clark-Flory, Tracy (February 17, 2013). "The "labia pride" movement: Rebelling against the porn aesthetic, women are taking to the Internet to sing the praises of "endowed" women.". Salon.com. Retrieved 2013-03-14.
- ↑ Sourdès, Lucile (February 21, 2013). "Révolution vulvienne: Contre l'image de la vulve parfaite, elles se rebellent sur Internet". Rue89. Retrieved 2013-03-14.
- ↑ Online Etymology Dictionary
- ↑ For slang terms for the vulva, see WikiSaurus:female genitalia — the WikiSaurus list of synonyms and slang words for female genitalia in many languages.
- ↑ Oxford English Dictionary. Oxford University Press.
Chiefly colloq. A girl or woman exhibiting characteristics associated with a cat, esp. sweetness or amiability. Freq. used as a pet name or as a term of endearment.
- ↑ A Dictionary of First Names (2nd ed.). Oxford University Press.
Pet form of Frances, very popular in the 18th and 19th centuries, but now much rarer.
- ↑ Silverton, Peter (2011). Filthy English: The How, Why, When And What Of Everyday Swearing. Granta Publications. p. 182. ISBN 978-1-84627-452-7.
- ↑ Rosewarne, Lauren (2013). American Taboo: The Forbidden Words, Unspoken Rules, and Secret Morality of Popular Culture. ABC-CLIO. pp. 81–82. ISBN 978-0-313-39934-3.
While pussy as a euphemism for vagina is very common in popular parlance, Mrs Slocombe was actually talking about her pet cat. In this context, the use of pussy works as a double entendre rather than as a euphemism.
- ↑ Jeffries, Stuart (2008). Mrs Slocombe's Pussy: Growing Up in Front of the Telly. Flamingo.
Mrs Slocombe's pussy changed all that.[...]It was funny, surely, because it dissolved that secret source of female power into a double entendre.
- ↑ "Yoni". Retrieved 30 March 2016.
- ↑ "Catherine Breillat, cinéaste", interview by Laurent Devanne, Radio libertaire (1 February 2004)
- ↑ McCartney, Jamie (2011). The great wall of vagina. Brighton: Jamie McCartney. ISBN 978-0956878502.
- ↑ "'The Great Wall Of Vagina' Is, Well, A Great Wall Of Vaginas (NSFW)". Retrieved 2016-04-17.
- ↑ Wheatstone, Richard. "Great Wall of Vagina: Vulva artist creates sculpture using plaster casts of women's private parts". Mirror Online. Retrieved 2016-04-17.
External links
| Look up vulva in Wiktionary, the free dictionary. |
 Media related to Vulvas at Wikimedia Commons
Media related to Vulvas at Wikimedia Commons Media related to Vulva symbols at Wikimedia Commons
Media related to Vulva symbols at Wikimedia Commons- 'V' is for vulva, not just vagina by Harriet Lerner discussing common misuse of the word "vagina"
- Vulvar hygiene and Urinary Tract Infections by Heather Corinna (illustrations; no explicit photos)

